MAKING THE DECISION TO HAVE YOUR IMPLANTS REMOVED DUE TO SILICONE BREAST IMPLANT ILLNESSES.
MAKING THE DECISION TO HAVE YOUR IMPLANTS REMOVED DUE TO SILICONE BREAST IMPLANT ILLNESSES.
Recently Danica Patrick, a former NASCAR car driver, opens up about illness she has attributed to her silicone breast implants. According to Danica, she got her breasts implant in 2014 because “she wants to have it all”. Like so many women in our early 20s and 30s, Danica admitted to having body image issues and has openly discussed it on her social media page. She was fit but “did not have boobs” and decided to have breast augmentation and for a while she loved them. However, “the wheels came off” 2 years ago when she noticed her menstrual cycle was irregular, weight gains, and her hair and skin changes. She got every clinical tests under the sun and listed her symptoms which included the following:
Hypothyroidism, heavy metal toxicity, dysiosis (gut imbalance); severe leaky gut, hypoglyemic, low estrogen, adrenal fatigue, swollen lymph nodes in her neck, and dizziness, achy hands, dry skin and scalp, and finally capsular contracture. She made the ultimately decision to have her implants removed. As documented on her social media page, she immediately feels better with “more energy and ability to take deeper breath.”
What Is “Breast Implant Illness” Or “BII”?
BII is used to describe a constellation of symptoms reported by some women following reconstruction or augmentation with breast implants.
They include, but are not limited to, fatigue, problems with memory or concentration (“brain fog”), joint and muscle pain, hair loss, rash,
inflammation weight changes and anxiety/depression. The appearance of such symptoms has been reported with all types of breast implants regardless of filling, shape or surface characteristic, and their onset anywhere from immediately after implantation to years later.
The largest retrospective cohort study examining connective tissue disease in relation to silicone breast implants published in 2018 by Conroneos et al., looked at over 99,000 women with silicone breast implants with a follow up period of 2-7 years. The study found statistically significant increased incidence of autoimmune/rheumatic disorders, Sjogren’s syndrome, systemic sclerosis, and sarcoidosis in women with silicone breast implants.
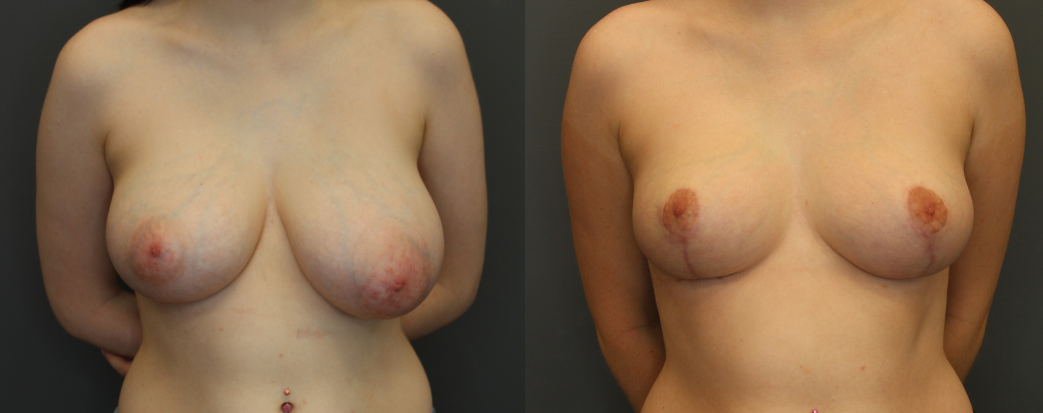
Many women after years of experiencing BII symptoms that no clinical tests or doctors could give an explanation for them, have decided to have their breast implants removed. It is a personal choice. When consulting a patient who has decided on removal of their breast implants, a plastic surgeon should council patients on the risks and benefits of breast implants explantation procedure as well as the physical defects often left following breast implant removal.
Breast implants removal involves not only removing the implant itself but also the removal of the capsule (scar tissue) that is formed around the implant.
Not all breast implants explantations are created equal. There are four different types of breast implant explantation.
- En bloc explanation – this is when the plastic surgeon leaves the capsule tissue intact on the breast implant and removes and capsule and implant as one unit. This is often performed through an incision on the inframammary fold of the breast because it allows for better visualization. More and more women seeking en bloc explantation for potentially less contamination of the silicone. Routinely, Dr. Goldberg performs en bloc explantation in ruptured implants or implants with thick calcified capsule.
- Explant with total capsulectomy – the plastic surgeon removes the implants and then removes all capsule tissue. This is not necessarily performed as one piece or en bloc fashion. This is the best option when the implants are very large which can be very difficult to perform as en bloc procedure.
- Explant with partial capsulectomy – the plastic surgeon removes the implants and then removes a portion of the capsule tissue. Often the posterior capsule on the chest wall is left behind due to the risks of injuring the lung or removal of the posterior capsule can result in chest wall deformity. This is rarely performed by Dr.Goldberg. It is only in rare instances whereby the capsule is densely adherent to the ribs and removing the capsule can potentially injure the lung creating pneumothorax.
- Open capsulotomy – capsule or scar tissue surrounding the implant is released surgically and left in the patient. As a rule, Dr. Goldberg does not leave behind the capsule when performing implant explantation.

In Cases Of ALCL Or Ruptured Implants With Thick Calcified Capsule, A Total Capsulectomy Is Mandated.
In writing this blog, Dr. Goldberg hopes to give women more information regarding breast implant illness and available up to date scientific data. If a woman chooses to remove her breast implants it is important to find a board-certified plastic surgeon with expertise in breast surgery and breast reconstruction. It is the job of the plastic surgeon to support his or her patient’s decision by providing up to date facts regarding health risks associated with silicone breast implants and the removal procedure.