WHAT ARE MY BREAST RECONSTRUCTION OPTIONS AFTER RADIATION?
WHAT ARE MY BREAST RECONSTRUCTION OPTIONS AFTER RADIATION?
6 Minute Read:
I received radiation treatment as part of my breast cancer treatment. What is the best breast reconstruction option for me: implant or autologous tissue breast reconstruction?
If you have received radiation as part of your breast cancer treatment, I hope this blog is informative for choosing the best option for your breast reconstruction.
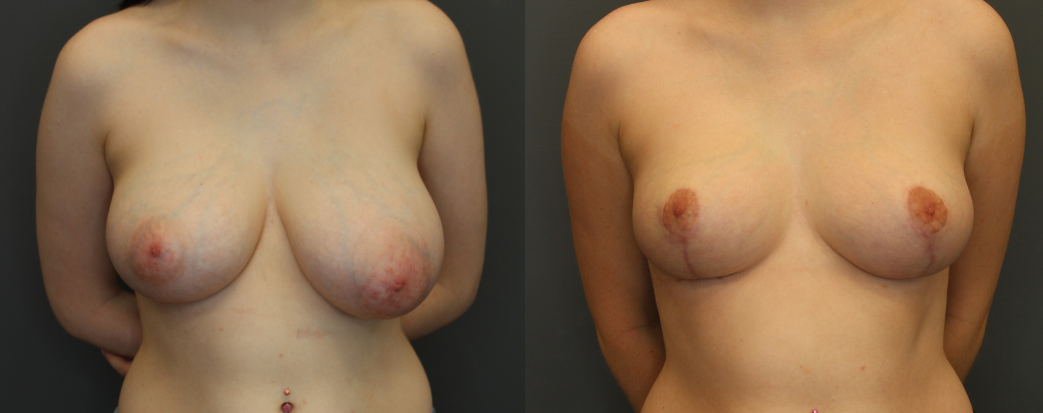
After mastectomy, the goal of breast reconstruction is to recreate an aesthetic breast mound plus or minus the nipple and to establish symmetry with the remaining breast.
WHAT IF I NEED RADIATION THERAPY?
Increasingly, radiation therapy is an important adjunct to breast cancer treatment. The current guidelines for post-mastectomy radiation include patients with breast cancer T3–4 disease and/or those with four or more positive axillary nodes. This therapy is performed because of its proven benefit in loco-regional control and overall survival.
Recent clinical trials on radiation treatment have even shown improvement in overall survival for patients with 1 -3 positive lymph nodes. Thus, more and more breast cancer patients receive post-mastectomy radiation as part of their breast cancer treatments.
WHAT DOES RADIATION DO TO THE BREAST TISSUE?
Although radiation therapy has beneficial effects on overall breast cancer survival, it has negative impacts on the chest wall and soft breast tissue.
Radiation causes damage at the DNA level, affecting the elasticity of the skin and impairing its healing ability.
Traditionally, breast reconstruction in patients who receive post-mastectomy radiation is delayed autologous breast reconstruction.
WHAT DO STUDIES SAY?
In recent years, implant reconstruction rates in the United States have risen in the irradiated patient population. A recent data analysis on immediate reconstruction trends among irradiated patients found a steady increase in implant-only reconstruction, from 27 percent to 52 percent. At the same time, there is a decrease in autologous tissue reconstruction in irradiated patients from 56 percent to 32 percent.
Even though the rate of implant-based breast reconstruction is on the rise, a large meta-analysis of the national database on patients receiving breast reconstructions showed significant high complication rates in implant-based reconstruction, especially in patients who have received post-mastectomy radiation. This included an overall failure rate of 20% and a 30% implant removal rate.
A clinical study titled, Reconstruction of the irradiated breast: A national claims-based assessment of postoperative morbidity. (M Chetta MD et. al. from University of Michigan, PRS, 139:783, 2017) assessed the morbidity associated with various breast reconstruction techniques in post-mastectomy radiated patients.
The study comprised of 4,781 irradiated patients who met the inclusion criteria. The majority of the patients [n=3846 (80%] received reconstruction with implants. The rest of the patients [n=935(20%] received autologous tissue reconstruction.
The overall complications rate in implant-based reconstruction was 45.3% for patients with implants and 30.8% for patients receiving autologous reconstruction.
Failure of reconstruction (complete loss of reconstruction) is 29.4% in patients with implant-based reconstruction compared with only 4.3% in patients with autologous reconstruction.
When adjusted for risk factors between the two groups of women undergoing breast reconstruction, implant base and autologous reconstruction, the study showed that patients who undergo implant-based reconstruction have twice the odds of having complications compared with those who underwent autologous reconstruction.
In addition, patients with implant-based reconstruction had 11 times the odds of complete failure of the reconstruction compared with women who underwent autologous reconstruction. The highest probability of reconstruction failure was among patients with implant-based delayed reconstruction and pre-reconstruction irradiation. The lower probability of failure of reconstruction was among patients with immediate autologous reconstruction with post-reconstruction irradiation.
Besides having an 11-folds increase in loss of reconstruction due to infection or implant extrusion, a significant number of women with chest wall radiation and implant-based breast reconstruction suffer from long-term capsular contracture, significant breast asymmetry, pain, and scar tissue.
Often patients with breast radiation and autologous tissue breast reconstruction were not discussed as an option during their breast reconstruction consult with a plastic surgeon. This is because the fact that their plastic surgeon does not offer autologous tissue or the false belief by many plastic surgeons that fat grafting or the use of ADM (acellular dermal matrix) prevents capsular contracture in irradiated patients. Scientific data does not support this belief.
WHAT SHOULD YOU DO BEFORE YOUR RECONSTRUCTION?
It is important to seek a consultation with a plastic surgeon who offers both implant and autologous tissue options for your breast reconstruction. He or she should discuss both the pros and cons discussed for both options during your consultation.
If you suffer from prolonged capsular contracture, breast asymmetry, or pain from implant-based breast reconstruction and wish to have your implant convert to your own natural tissue, autologous tissue breast reconstruction is the best option. With the advancement in microsurgery in recent years, we are now able to offer a variety of options for autologous tissue reconstruction besides the DIEP flaps. These options include the lower back (lumbar perforator (LP) flap, profunda artery perforator (PAP) flap, superior gluteal artery perforator flap (SGAP), and upper back thoracodorsal perforator flap (TDAP). We are embarking on a new era of microsurgery breast reconstruction whereby we tailor our reconstruction options according to the patient’s body habitus (available tissue). It is no longer a prolonged surgery but a relatively fast surgery with a minimal recovery period. The results from autologous tissue reconstruction are long lasting, aesthetically beautiful, and natural.
CONTACT DR. GOLDBERG FOR YOUR BREAST RECONSTRUCTION
Dr. Mytien Goldberg is a leading female plastic surgeon in Beverly Hills who specializes in breast reconstruction and breast reconstruction revision. Recognized by her peers as one of the most skilled microsurgeon, she is also known for her attention to detail, high-caliber surgical skills, and beautiful, natural results. For women seeking breast reconstruction or breast reconstruction revision, Dr. Goldberg offers a wide spectrum of flap reconstruction using different parts of your body to recreate natural breasts, including DIEP, SGAP, PAP, LAP flaps and hybrid reconstructions. She has been in practice for over 10 years and is a faculty member with the division of plastic surgery at UCLA David Geffen School of medicine. She was awarded the teacher of the year by UCLA chief residents for her mentorship and teaching.
If you are recently diagnosed with breast cancer and are looking for a plastic surgeon to perform your breast reconstruction, Dr. Goldberg is your plastic surgeon. And if you have had breast cancer and are dissatisfied with your reconstruction results, the first step is to schedule a comprehensive in-office consultation with Dr. Goldberg. After the exam, Dr. Goldberg can create an individualized plan to address your specific concerns and answer any questions you may have.
For many women in southern California and around the country, Dr. Mytien Goldberg is the plastic surgeon of choice for breast reconstruction, revision, and correction procedures.